Many of you asked, so here’s my current take on Omicron.
Why have I not written earlier1? For me, analysis must drive to action. If analysis is not actionable, it doesn’t really matter.
There’s been a lot of great coverage of Omicron so far, but with the data we have, we can’t change our behavior at all. It’s not actionable. We’re missing one fundamental piece of information. It’s the Omicron question. This article will look at what we know so far to zero in on that big question.
There are two numbers that matter in epidemiology: the transmission rate and the fatality rate2. The transmission rate tells you how many people are likely going to catch a virus, and how hard it will be to fight it. Once you catch it, the fatality rate tells you how bad it will be.
There’s an additional factor that matters: The Scary Virus Paradox. There’s an interaction between these two: a virus with high transmission rates but low fatality rates might end up killing more people than if the virus has higher fatality rates.


The accepted wisdom was originally that “when the transmission rate increases, the fatality rate tends to decrease, because a virus can only spread more if it doesn’t kill its host too fast”.
I explained how this was unlikely to be true with Alpha:


And it happened again with Delta. The transmission and fatality rates increased because both were caused by the same factor: an improvement in the spike protein that allowed them to infect cells better. Better infection meant easier infection, faster reproduction in the body, faster infectiousness towards other people, more intense infectiousness, stronger symptoms, higher hospitalization rate, higher fatality rate, and a death that came sooner.
It didn’t reduce the virus’ transmission rate when death came sooner, because by the time a person dies, she’s usually been isolated for some time, so the reduction in life after infection didn’t reduce the time during which the sick person was infectious. Put in another way: if you’re isolated in the hospital, it doesn’t matter to the virus’ spread whether you take 2 days to die or 2 years.
As long as the mutations of the virus were limited to a few changes in the spike protein, the most likely outcome was that this would continue to happen: better penetration into cells meant a higher transmission rate and higher fatality rate.
We’ve known this for ages in immunology. It’s called passage.
And this is the wild card of Omicron.
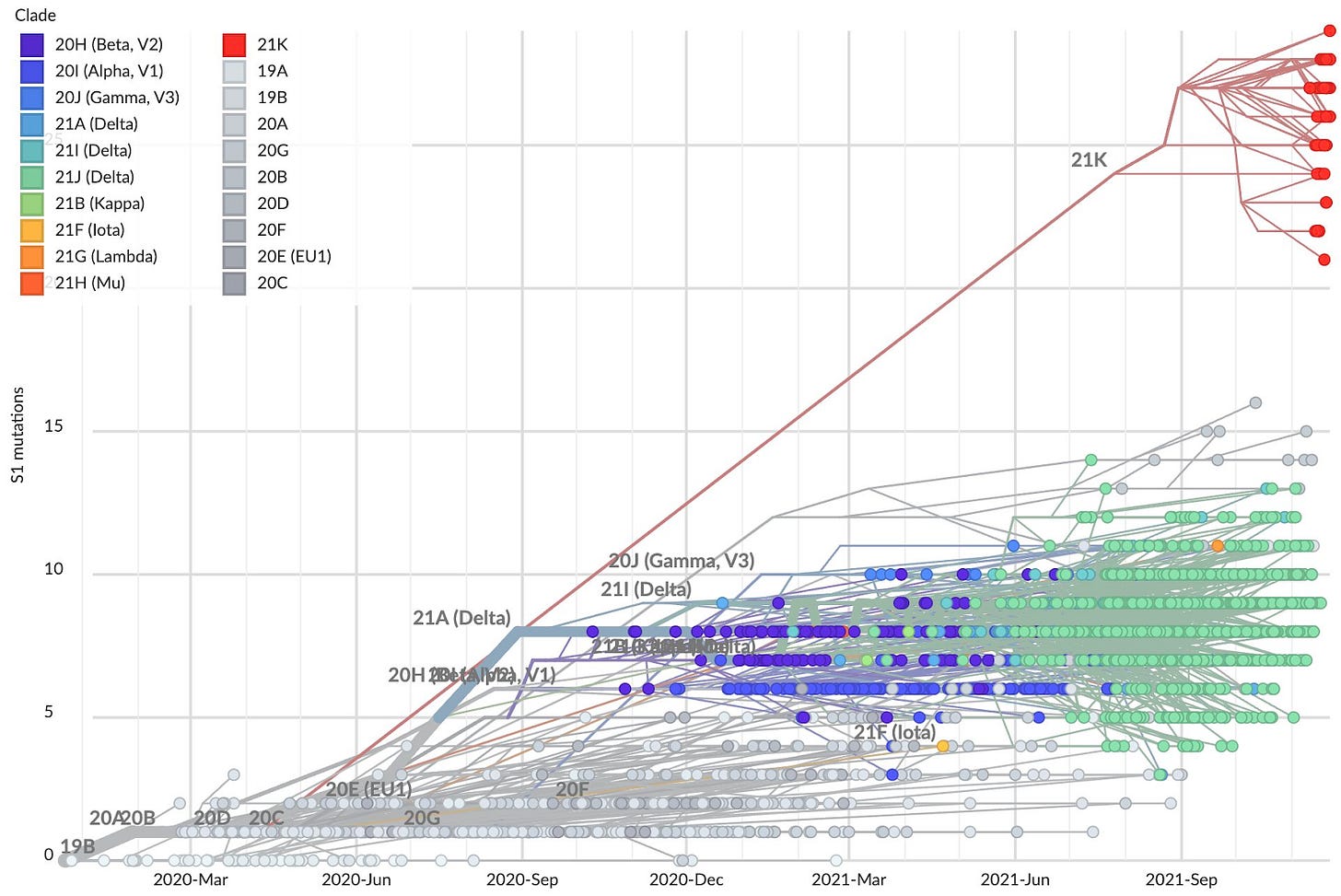
Alpha, Delta, and most other variants of concern were just optimizations of each other, as seen by the progressive evolution of mutations in the blue/green on the lower right.
Omicron is not yet another optimization. In fact, it might have evolved from the early variants, independently from the evolution of the last few months.

So many independent mutations make it a wild card. It could become more transmissible, but maybe the mutations inside the spike protein or in other places could cause the virus to be less lethal. Maybe there’s something else.
And there’s hope, because historically, this is how viruses tend to evolve. Early on, they might become more transmissible and lethal, but as time passes, they become just more transmissible and less lethal. This is what has happened with the flu and cold viruses. This is what happened to the 1918 flu.
The first wave was mostly mild. It spread from Kansas to the rest of the world, tagging along with the military during WW1. It killed a few people. Most recovered. But by the time the second wave hit at the end of 1918, it was a bloodbath. The virus likely evolved to be more transmissible and lethal, annihilating its hosts. Alpha and Delta did the same thing compared to the original variant: higher transmission and fatality rates.
But the 3rd and last wave was milder, and then the virus disappeared, likely evolving into the H1N1 strain we know today—the same one that caused the Swine Flu of 2009.
Why was that 3rd wave weaker? It might have been a combination of more immunity from the population and weaker lethality of the virus. We’re not sure. The most likely reason is because H1N1 killed too fast. It needed to become milder to spread further.
Omicron is unlikely to have suffered that natural selection, but because it’s so mutated, and so independently from other variants, it’s a wild card. It appears to have a higher transmission rate and lower fatality rate. Is that true? If so, is that because the virus is less lethal? Or because of more acquired immunity in humans? Let’s try to figure it out.
Omicron by the Numbers
Omicron’s Transmission Rate
You can’t stop it.
Delta’s R03 is between 4 and 9 (let’s assume 6 for simplicity). Remember that R0 is in the absence of any measures (like masks) or acquired immunity (like vaccines or previous infections). When the Delta wave subsided, it meant that measures plus acquired immunity had pushed Delta’s R0 of ~6 to an Rt below 1, for a ~85% reduction in Rt.
So where does that put Omicron’s R?
But that’s just Gauteng. Now we know from other places too:
It appears that the higher transmission rate of Omicron is confirmed across countries, with the UK and Germany indicating much higher Rts than for Delta.
In South Africa’s Gauteng region, Rt was 3-4 times higher in Omicron than Delta, which would place Omicron’s R0 at 16-30. Put another way: every infected person would infect 16-30 other people. This would be among the most infectious diseases we’ve ever seen. Unlikely.
Does Omicron simply have a much larger R0? Or is there something else? Maybe it’s simply escaping current immunity better. Maybe those protected from Delta thanks to previous infections and vaccines were the reason why the transmission rate was lower.
We’re not sure. If Delta’s R0 is 6, an explanation for Omicron’s growth might be that it has about 40% escape from current immunity. Or it could have an R0 of 9 and 20% escape immunity. Or an R0 of 3 and above 80% escape.
One reason to suggest that R0 is on the high side is that in South Africa, it has spread so fast that cases might already be going down due to increased acquired immunity.
But the community thinks R0 is in fact similar to Delta’s.
This is from a prediction market called Metaculus. Prediction markets aggregate the knowledge of everybody who votes. Research shows that people’s errors cancel each other out, so the average of everybody’s opinions tends to aggregate the information that everybody has, and tends to be accurate. Here, the community believes that Omicron’s R will be close to 6, so similar to Delta’s.
If Omicron’s R0 is indeed 6, but it’s growing three times faster than Delta, immune escape must be quite high. So is it?
Omicron’s Immune Escape
One clue we have is the sheer number of mutations. This should escape immunity much better than previous variants. Is that what we are seeing?
In labs, at least, it is. Having caught COVID in the past or being vaccinated didn’t help nearly as much with Omicron as with Delta. From a pre-print:
This result has been repeated in other studies.
One thing to note is that lab results don’t translate perfectly to contagiousness. You can have 30 times fewer antibodies, but you won’t be 30 times less protected. The relationship between these two numbers is not direct at all, and we’re not sure what they will mean for the likelihood of infection for vaccinated people. With Delta, for example, we knew that vaccines reduced your chances of infection by 50% and of death by 90%. Vaccination still helps tremendously, though, so we should continue doing it and getting a booster shot if we can.
One of the questions we can ask is: why suddenly so much immune escape?


If most people are either infected or vaccinated—as is the case in South Africa—a new winning variant is not going to be the one tweaking its transmission rate in an unprotected population. The winning variant will be the one bypassing existing immunity the most, even at the cost of some transmission rate reduction in unprotected people.
If 90% of people are not immune yet and 10% are, as a virus you want to optimize for those not immune yet. But if it’s the opposite, and now 90% of people are immune, you’ll switch your efforts and evolve to increase your transmission rate among immune people.
This is what a South African study found. Uninfected people (called “naive”) were less likely to be infected by Omicron than with Delta, but those with a previous infection were more likely to be infected.
Do we have any data to tell how much immune escape there is? It’s starting to arrive.

How to interpret this graph: the black line was the effectiveness of Delta against vaccines (here, Pfizer. Others follow the same trends). As you can see, six months (25 weeks) after the second dose, effectiveness was about 60%, which meant that you were 60% less likely to get infected if you had 2 doses than if you weren’t vaccinated. This is for catching the virus. The reduction in hospitalization and death was even better.
Now compare that to Omicron, in blue. We’re not sure yet about the vaccine effectiveness (hence the blue area instead of a blue line) but it looks like the effectiveness at stopping infections could go down from ~60% with Delta to ~30% with Omicron. Now, again, this is just for infection. Protection for death is probably much higher. But how much?
Omicron’s Fatality Rate
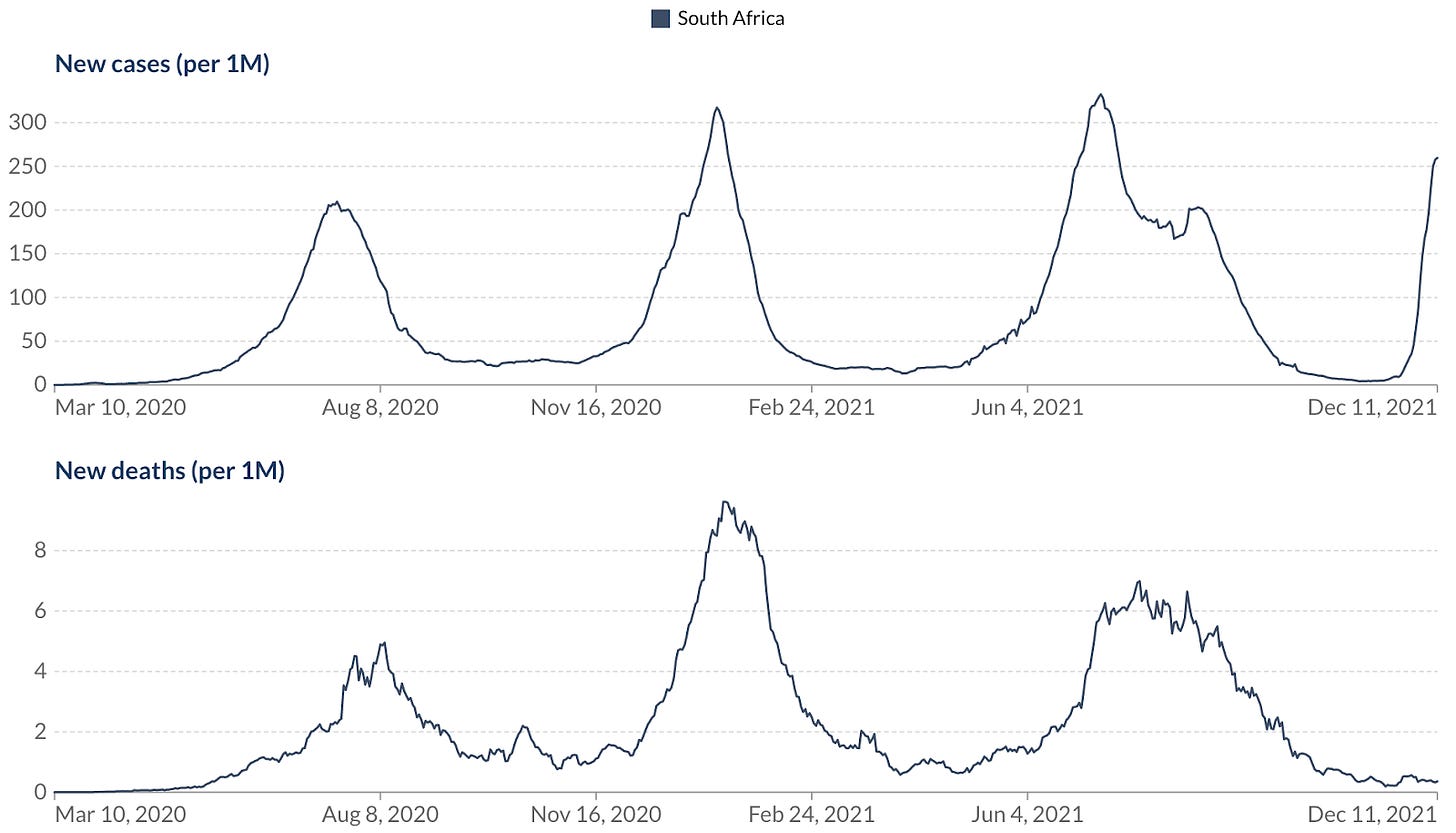
Cases are peaking in South Africa overall, but deaths are not following yet.
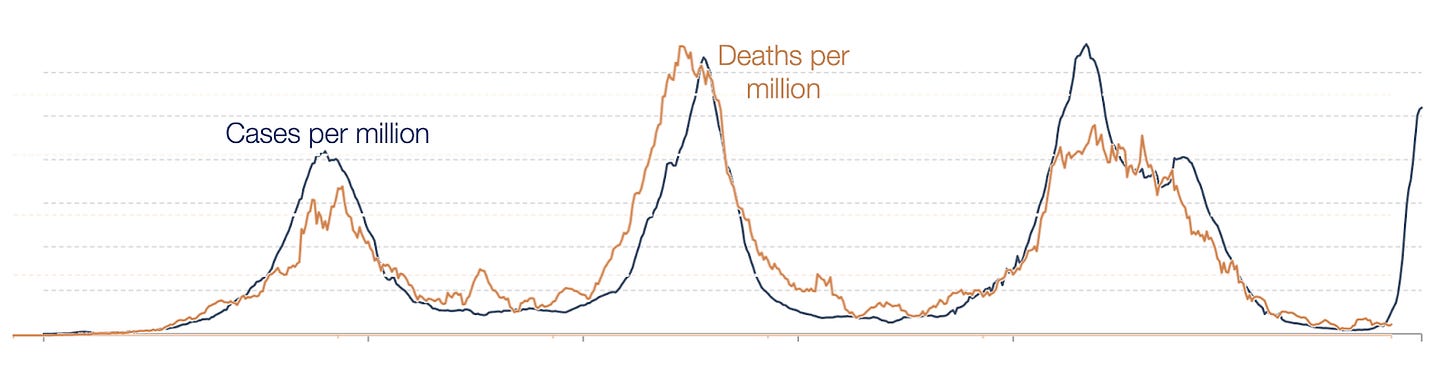
Is it just a matter of delay? Let’s superimpose the graphs to see. In the graph below I took the two graphs above and pulled the deaths (now in brown) forward a few weeks so they overlap with cases.
So far, no deaths. That’s good. But we’re about the time when we should start seeing them. They’re very likely to go up. The question is not whether, it’s how much.
Since we can’t look at deaths directly, we need to look at other proxies: hospitalizations, opinions from people on the ground… Let’s look at them. First, hospitalizations. They are indeed climbing up. Too early to tell by how much.
Another data point: the share of positives that require ICU support.
Across all ages—except 20-30 years old4—the share of people who need the ICU is much lower for Omicron than Delta. Fantastic.
This has been true over time. And we also see it in the need for ventilators.
This is even better. The closer you get to death, the more relevant it is to predict deaths. If the share of people needing ventilators with Omicron is 75% lower than for Delta, it might mean that deaths go down by about that amount.
The problem with this data is that when the Delta wave hit South Africa, less than 1% of the population had been vaccinated. By the time it ended, about 25% of people were. With fewer vaccinated people, we should expect more deaths. So is Omicron sending less people to the ICU because it’s less lethal, or because more people are vaccinated or have immunity from previous variants? The only way we could tell is if we had data on fatality rates of Omicron vs. other variants separated by vaccinated, previously infected, and naive.
Let’s see what the community forecasts for fatality rates:
People believe that there’s only a 15% chance that Omicron will be deadlier than Delta. Good.
We know anecdotally that doctors report milder symptoms.
A video from a South African doctor:

But is this because the virus is milder, or because everybody has immunity from Delta? Or because more people are vaccinated? This matters, because we’re only halfway through in vaccinating the world.
Other Important Factors
Vaccinations Fall Short
Nearly 60% of the population is now vaccinated. That’s great, but not enough for Omicron. It still leaves 40% of the global population without a single vaccine dose.
We don’t know whether that remaining 40% has mostly been exposed to the virus in the past or not. If 35 percentage points of those 40 have been naturally infected, and previous infection protects heavily against death, then we should be good. The opposite situation would drive a global Omicron wave the size of Delta in India.
I’m optimistic. I assume Delta has been circulating pretty freely around the world already. Increases in vaccinations will simply improve our immunity.
Transmission vs. Fatality Rates
One more word about transmission rates vs. fatality rates. There’s this common theme that “a virus that is less lethal but more transmissible will kill more”, consistent with the Scary Virus Paradox. Indeed, if you kill 20% less but you’re 20% more transmissible, because transmissions are exponential, you end up with many many more people infected, and hence many more deaths.
That assumes, however, that these viruses don’t reach saturation. This is probably not the case here. With such a high transmission rate and immune escape, this virus will likely reach everywhere, similar to Delta. That’s why Omicron selected for immune escape in the first place.
If virus A is 20% more transmissible than virus B, but both are transmissible enough that they will infect everybody, then the transmission rate doesn’t matter. You’d rather look at the fatality rates to see how many people are going to die in total.
Long COVID
There’s also another wild card here. Long COVID affects about 2-3% of those infected with COVID. How will that evolve? Will it be comparable to the fatality rate? Would a lower fatality rate mean a lower rate of Long COVID? Or could it be the opposite?
Unfortunately, I don’t think we’ll know this until a few months after Omicron’s waves, so we need to guess. I have no idea how to think about this. I want to believe that a milder virus doesn’t cause Long COVID as much, as I’ve never heard of people who get Long COVID from a cold. It tends to be more dangerous viruses like mononucleosis / Epstein-Barr or HPV6. But I don’t know. For lack of more data than this, I’ll just use this rule of thumb to hope Long COVID is milder for Omicron.
Conclusion
If you haven’t had COVID before, you’re going to get it.
You can only escape it while you lock yourself out. The moment you come back into society, you will get exposed to it. Paradoxically, this can be good.
This is the final battle for COVID. It’s throwing everything it has at us and will overwhelm the world. But in doing so, it might have weakened itself. And it’s attacking at a moment when the world is well-armed with vaccines and prior infections.
In this final battle, many people will die. But they might be few in comparison to what it could have been.
This all hangs on one data point, the Omicron Question: the fatality rate
With vaccines
With previous infection
Without vaccine or previous infection
It will take us a few weeks to get that data. Only when we get that will we be able to tell if Omicron is good or bad. I’m hopeful based on anecdotal evidence and community prediction, but we just don’t know. If you find research that can inform us, please share it with me.
In the meantime, I’ll get my booster shot, mix-and-match it, get my N955 masks back out, avoid massive indoor parties, and vaccinate my kids. Which is what I was going to do anyway.
Hopefully we’ll emerge on the other side of this wave in a world where our immunity to COVID is so strong that we don’t need to worry about it beyond getting our booster shots every now and then.
Take care.
If you want more of this analysis, subscribe to this newsletter. I apply the same approach to everything I analyze, from what China wants, to the end of nation states.
I’ve been silent on Omicron for many reasons besides actionability.
First, the appearance of a new, more transmissible variant is not really news. We’ve had new variants of interest for a year now. The ramifications of Alpha were something we quickly needed to understand better, and the world was not reacting fast enough, so I wrote about it. The world expected the fatality rate of Alpha to be lower, so I explained why that was unlikely to be the case. People didn’t understand the story was repeating with Delta, so I wrote about it. People didn’t take Long COVID into consideration, so I did.
Second, many amazing analysts have been extremely fast at reporting accurate information about COVID in general and Omicron in particular. You can get great articles about it, for example here, here, here, and here.
Third, at this point there are more important problems in the world to pay attention to.
There are also important secondary numbers, such as the rate of long-term consequences, like Long COVID, for example.
R0 is R (the transmission rate, the “reproduction number”) at time 0, initially, when there are no measures and no immunity, when everybody is immunologically naive. Rt is R but at a moment “t”, later on, once there are measures and immunity from vaccines and things like that. We tend to use it as “the R today”. So Rt is usually the transmission rate today, and it’s compared to the R0 of the original variant.
Maybe an artifact of too little data?
N95 vs. surgical masks is a cost-benefit question. If it costs you nearly the same to wear N95 masks, or if that cost doesn’t matter to you much (in terms of money or inconvenience), then you should totally use N95s. But use them judiciously: no need outdoors, for example. Of if you’re alone. Or if you’re about to have dinner in a restaurant without a mask for 2 hours and just put it back up to exit.



















Good analysis in the later portion of the article. However, you omitted the more recent preliminary finding that suggests WHY the mortality rate is lower in Omicron.
> Omicron SARS-CoV-2 can infect faster and better than Delta in human bronchus but with less severe infection in lung <
https://www.med.hku.hk/en/news/press/20211215-omicron-sars-cov-2-infection
I take issue with the proposition that nothing is "actionable." I subscribe to the PHYSICAL BARRIER solution as 99.9% protection from unsanitary humans who simply cannot help but spit on each other.
https://doi.org/10.1371/journal.pcbi.1009629
It really is that simple -- "build a wall" and stop every variant & strain from immigrating to the body-nation. However, I am an engineer with clean room experience, and I am quite aware of the movement of particles which I cannot see. Most people can't even keep fecal particles off their toothbrush.
For example, at NIH Clinical Center; Bethesda, MD, Ebola "magically" spread to a completely separate wing. Yet a Frontline documentary plainly showed staff entering and exiting the "contaminated zone" without even cleaning the soles of their shoes or the wheels on carts. In my opinion, the pandemic is ultimately the result of human ignorance, arrogance, and unwillingness to track the spread of human filth. Only the "vaccine" of both intellectual and emotional education can cure that. See e.g., https://ycei.org/
I wear a P100 respirator, and goggles. Respirator body cost $23 on Amazon (3M 6500 series), and the filters cost $8-12 on ebay (3M 7093 or 2291). The filters last about 6-8 months, since I am not in a "dusty" environment. I.e., use them until the airflow is unacceptably reduced or "clogged." Also, the respirator is designed to be worn every work day, all day, and is an order of magnitude more comfortable than disposable masks. Don't even get me started about "surgical" style masks, which a recent study found to be equivalent to N30, due to significant leakage.
Note: filtration media degrades as moisture causes the material to clump together. Thus, a bidirectional N95 mask has a much shorter life span than a unidirectional respirator filter.
I also routinely disinfect hands with hydrogen peroxide or benzalkonium chloride, particularly when transitioning between isolated and exposed locations. Yes, I even pour H2O2 on the ground and clean the soles of my shoes. Even wiping down the surfaces of a grocery cart, I clean parts of the handle that are NEVER cleaned by anybody, and remove black "gunk."
Another masterful presentation of information using clear visuals. Thanks for writing this piece. The ICU and ventilation data from S. Africa are encouraging, with the caveat that many of those infected thus far are young and therefore unlikely to experience severe symptoms. I do want to comment on your description of the virus' evolution, as in "If 90% of people are not immune yet and 10% are, as a virus you want to optimize for those not immune yet. But if it’s the opposite, and now 90% of people are immune, you’ll switch your efforts and evolve to increase your transmission rate among immune people." Just to be clear, evolution is not teleological; the virus doesn't have a master plan for how to infect the greatest number of people. Evolution occurs through random processes of mutation and natural selection. Changes in the nucleotide sequence of DNA or RNA occur randomly during replication; as a rough rule of thumb, a mistake in one or more nucleotides occurs about 1 out of every 100,000,000 times the DNA/RNA is copied, each of which can lead to a mutation. Most changes are neutral or deleterious to the virus, but some mutations are beneficial (for the virus) by increasing its ability to enter host cells, spread between cells, evade host antibodies, transmit between hosts, and so on. If a new virus variant has one or more beneficial mutations, it may spread rapidly through a host population and out compete other variants that lack its advantages. This is what seems to be occurring with omicron. This is a purely random process. The virus isn't trying to reach a goal point, its only "purpose" is to replicate itself in the cells of a host. We face the challenge of responding to new mutations as they arise, with no early warning system as to the nature of those mutations. Fortunately, we have good defenses in vaccination (with booster), masking, and distancing when necessary.